
Threats to Global Health –
The world is facing multiple health challenges. These range from outbreaks of vaccine-preventable diseases like measles and diphtheria, increasing reports of drug-resistant pathogens, growing rates of obesity and physical inactivity to the health impacts of environmental pollution and climate change and multiple humanitarian crises.
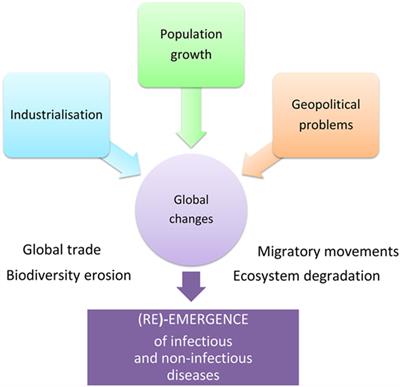
Global health plays an increasingly crucial role in global security. As the world and its economies become increasingly globalized, including extensive international travel and commerce, it is necessary to think about health in a global context. Rarely a week goes by without a headline about the emergence or re-emergence of an infectious disease or other health threat somewhere in the world.
The health of the global population can be affected by public health threats or events across the globe. Recent examples of this include the outbreak of coronavirus from china, the Ebola Virus outbreak that began in 2014, the 2009 spread of novel H1N1 influenza, and the 2003 SARS epidemic. Improving global health can support national and global security interests by fostering political stability, diplomacy, and economic growth worldwide.
Click here for Emerging Issues in Global Health –
Globally, the rate of deaths from non-communicable causes, such as heart disease, stroke, and injuries, is growing. At the same time, the number of deaths from infectious diseases, such as malaria, tuberculosis, and vaccine-preventable diseases, is decreasing. Many developing countries must now deal with a “dual burden” of disease: they must continue to prevent and control infectious diseases, while also addressing the health threats from non-communicable diseases and environmental health risks. As social and economic conditions in developing countries change and their health systems and surveillance improve, more focus will be needed to address non-communicable diseases, mental health, substance abuse disorders, and, especially, injuries (both intentional and unintentional). Some countries are beginning to establish programs to address these issues like India.
The most important health problems – When thinking about the most serious health problems, there are several ways of looking at them. For example, you might consider
- the most common causes of death
- the diseases and conditions of death people worry about the most
- the causes of death that are somewhat unique to where you live.
These three lists are not the same. Let’s consider each.
The top health problems in the world today :
- Heart Disease – Smoking, high-fat diet, lack of exercise, and a sedentary lifestyle are common causes, while other body conditions add fuel to the fire aggravating the disease. Atherosclerosis, diabetes, hypertension, and infections are common culprits.
Preventive measures like putting an end to smoking, minimizing salt intake, regular physical exercise, consuming a diet low in fat, and having regular health checkups will do a lot in reducing your risk for heart diseases.
- Cancer – While there’s no particular cause of cancer, various risk factors contribute to the genesis of particular kinds of cancer. Tobacco and smoking, obesity, alcoholism, too much sun exposure, and radiation are among the common risk factors, while genetics also plays a pivotal role with increased risk among siblings and relatives.
Regular screening for cancer, lifestyle modifications like regular exercise, healthy diet, quitting smoking, and tobacco are preventive measures.
- Extreme Obesity – Increasing obesity rates are not just limited to traditionally wealthy countries but its seen globally. Obesity has been described as an epidemic in modern society. The Obesity problem may be the world’s next great challenge. Being obese causes a variety of health-related issues, increasing your risk of diabetes, heart disease, stroke, and many other problems.
Experts put the explosion in obesity rates in the last decade down to an increase in caloric intake, rapid urbanization, and the rise of new technology that promotes sedentary lifestyles. The impact is felt particularly hard in populations where exercise is not a defining part of the culture. There have been some great advancements in nutritional science in the last few decades. An understanding of food and how it affects hormones in the body have led to the spread of better information about nutrition.
- Aids – Transmitted through body fluids–blood, semen, breast milk, vaginal fluid, rectal fluids—it can be prevented if transmission of fluids can be avoided. Hence, safe blood transfusion, safe sex, limiting the number of sexual partners, getting tested and treated for other STDs are effective preventive measures.
Antiretroviral therapy (ART) helps HIV infected people to minimize virus load and stop the progression of disease thus, reducing the risk of transmission to other people as well.
- Stroke – Stroke or cerebrovascular accident is a condition potentially caused when blood supply to the brain is interrupted thus leading to the death of brain cells. It may be caused by ischemia– due to the blocked artery—or it can be hemorrhagic—due to the bursting of the blood vessels. Risk factors include obesity, physical inactivity, hypertension, and diabetes, while genetics also plays a role. Since it can lead to a number of complications like paralysis of contralateral sides of the body, loss of cognitive function, emotional problems and abnormal behaviors, and also due to the fact that treatment for any disease of the brain is complicated, one ought to have adequate knowledge about stroke, about its risk factors in general and everyone should develop a healthy lifestyle.
- Alzheimer’s disease – While the exact cause of Alzheimer’s disease remains unknown, it’s widely known that advancing age and family history are common risk factors along with obesity, hypertension, and Down syndrome among others.
Treatment therapy includes only symptomatic therapies–cholinesterase inhibitors. Drugs are used according to symptoms, like antidepressants for depression and for agitation, sleep disorders, etc. Routine physical exercise will have an effect on disease progression as increased cardiorespiratory fitness has been shown to slow disease progression.
- Diabetes – Diabetes is a chronic condition associated with abnormally high blood glucose levels: fasting blood sugar level greater than 110 mg/dl, random blood glucose level greater than 200 mg/dl.
Preventive measures include lifestyle modifications like regular exercise, the inclusion of fiber-rich whole grains, nuts, vegetables and fruits in diet, maintaining a normal weight, and regular checkup.
- Influenza – Immunocompromised people, especially children, old, pregnant women, and people with conditions like diabetes and hypertension are at increased risk of developing potentially fatal pneumonia.
With complications like pneumonia, influenza poses a serious threat, especially to the above-mentioned risk groups. Preemptive vaccination is the most effective way to prevent disease while regular washing of hands, preventing unnecessary touching of nose and mouth, and wearing masks are also to be followed. Hence, necessary precautions and prevention are the most efficient way to save oneself from falling victim to the influenza virus.
- Kidney Disease – Causes of acute kidney injury include pre-renal causes like dehydration, blood loss, and shock; renal causes include infections of the kidney; obstruction to urine flow falls under post-renal causes.
Guidelines for kidney disease prevention include reduced protein intake, salt restriction, adequate fluid intake, cessation of smoking, and maintaining normal body weight.
- High Blood Pressure – High blood pressure impacts numerous other body systems and people with high blood pressure are more likely to develop coronary heart disease, stroke, heart failure, peripheral vascular disease, kidney failure, and certain eye conditions.
- Smoking and Tobacco – Smoking harms nearly every organ in the body. It increases your risk of cancer, diabetes, heart disease, lung disease, and stroke. If you smoke you are more likely to catch tuberculosis, develop certain immune disorders such as rheumatoid arthritis, and have erectile dysfunction.
Bottom line: If you don’t want to die prematurely; don’t smoke and don’t eat tobacco in any form..
Contrast the list above to the health concerns that rise to the top when large numbers of people are surveyed. As for diseases, here are the most frequently mentioned concerns:
- Obesity:
- Cancer:
- Diabetes:
- Drug & alcohol abuse:
- Heart disease:
- Flu:
- Mental illness:
- AIDS:
Remarkably, many of the top causes of death don’t even show up on this list, and many that do barely register. Perhaps survey respondents are thinking more about conditions that cause suffering or impaired quality of life rather than causing death. Or, perhaps the causes of death that primarily affect the elderly (such as stroke) are not as big a concern to the public as those that affect younger individuals. Whatever the reason, the difference is striking.
Why it Matters – It’s not surprising that the top causes of death might vary from country to country. But, that means that the measures we should take to improve our health may not be the same everywhere. It’s particularly important to recognize those diseases that we know can be prevented, slowed, or even reversed with preventive care, changes in diet, exercise, or medications. Good examples include many cases of diabetes and heart disease.
While avoiding preventable death is an important measure of health, it’s not the only one. Maintaining a high quality of life matters as well — and some would say that quality of life is more important than how long it is. Still, information about causes of death is of interest not only because of what it may say about how we live but also in directing interventions.
Click here for Issues requires attention from WHO –
Here are a few of the many issues that will demand attention from the WHO and the Health Department.
Air Pollution and Climate change – Nine out of 10 people breathe polluted air every day. In 2019, air pollution is considered by the WHO as the greatest environmental risk to health. Microscopic pollutants in the air can penetrate respiratory and circulatory systems, damaging the lungs, heart, and brain, killing 7 million people prematurely every year from diseases such as cancer, stroke, heart and lung disease. Around 90% of these deaths are in low- and middle-income countries, with high volumes of emissions from industry, transport, and agriculture, as well as dirty cookstoves and fuels in homes.
The primary cause of air pollution (burning fossil fuels) is also a major contributor to climate change, which impacts people’s health in different ways. Between 2030 and 2050, climate change is expected to cause 250 000 additional deaths per year, from malnutrition, malaria, diarrhea, and heat stress.
In October 2018, WHO held its first-ever Global Conference on Air Pollution and Health in Geneva. Countries and organizations made more than 70 commitments to improve air quality. In 2019, the United Nations Climate Summit in September aimed to strengthen climate action and ambition worldwide. Even if all the commitments made by countries for the Paris Agreement are achieved, the world is still on a course to warm by more than 3°C this century.
Non Communicable disease – Non-communicable diseases, such as diabetes, cancer, and heart disease, are collectively responsible for over 70% of all deaths worldwide, or 41 million people. This includes 15 million people dying prematurely, aged between 30 and 69.
Over 85% of these premature deaths are in low- and middle-income countries. The rise of these diseases has been driven by five major risk factors: tobacco use, physical inactivity, the harmful use of alcohol, unhealthy diets, and air pollution. These risk factors also exacerbate mental health issues, that may originate from an early age: half of all mental illness begins by the age of 14, but most cases go undetected and untreated – suicide is the third leading cause of death among 15-19 year-olds.
Among many things, this year WHO will work with governments to help them meet the global target of reducing physical inactivity by 15% by 2030 – through such actions as implementing the ACTIVE policy toolkit to help get more people being active every day.
Global influenza Pandemic – The world will face another influenza pandemic – the only thing we don’t know is when it will hit and how severe it will be. Global defenses are only as effective as the weakest link in any country’s health emergency preparedness and response system.
WHO is constantly monitoring the circulation of influenza viruses to detect potential pandemic strains: 153 institutions in 114 countries are involved in global surveillance and response.
Every year, WHO recommends which strains should be included in the flu vaccine to protect people from seasonal flu. In the event that a new flu strain develops pandemic potential, WHO has set up a unique partnership with all the major players to ensure effective and equitable access to diagnostics, vaccines, and antivirals (treatments), especially in developing countries.
Fragile and vulnerable settings – More than 1.6 billion people (22% of the global population) live in places where protracted crises (through a combination of challenges such as drought, famine, conflict, and population displacement) and weak health services leave them without access to basic care.
Fragile settings exist in almost all regions of the world, and these are where half of the key targets in the sustainable development goals, including on child and maternal health, remain unmet.
WHO will continue to work in these countries to strengthen health systems so that they are better prepared to detect and respond to outbreaks, as well as able to deliver high-quality health services, including immunization.
Anti Microbial Settings – The development of antibiotics, antivirals, and antimalarials are some of modern medicine’s greatest successes. Now, time with these drugs is running out. Antimicrobial resistance – the ability of bacteria, parasites, viruses, and fungi to resist these medicines – threatens to send us back to a time when we were unable to easily treat infections such as pneumonia, tuberculosis, gonorrhea, and salmonellosis. The inability to prevent infections could seriously compromise surgery and procedures such as chemotherapy.
Resistance to tuberculosis drugs is a formidable obstacle to fighting a disease that causes around 10 million people to fall ill, and 1.6 million to die every year. In 2017, around 600 000 cases of tuberculosis were resistant to rifampicin – the most effective first-line drug – and 82% of these people had multidrug-resistant tuberculosis.
Drug resistance is driven by the overuse of antimicrobials in people, but also in animals, especially those used for food production, as well as in the environment. WHO is working with these sectors to implement a global action plan to tackle antimicrobial resistance by increasing awareness and knowledge, reducing infection, and encouraging prudent use of antimicrobials.
Ebola and other high threats pathogens – In 2018, the Democratic Republic of the Congo saw two separate Ebola outbreaks, both of which spread to cities of more than 1 million people. One of the affected provinces is also in an active conflict zone.
This shows that the context in which an epidemic of a high-threat pathogen like Ebola erupts is critical – what happened in rural outbreaks in the past doesn’t always apply to densely populated urban areas or conflict-affected areas.
At a conference on Preparedness for Public Health Emergencies held last December, participants from the public health, animal health, transport, and tourism sectors focussed on the growing challenges of tackling outbreaks and health emergencies in urban areas. They called for WHO and partners to designate 2019 as a “Year of action on preparedness for health emergencies”.
WHO’s R&D Blueprint identifies diseases and pathogens that have the potential to cause a public health emergency but lack effective treatments and vaccines. This watch list for priority research and development includes Ebola, several other hemorrhagic fevers, Zika, Nipah, Middle East respiratory syndrome Coronavirus (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS) and disease X, which represents the need to prepare for an unknown pathogen that could cause a serious epidemic.
Weak Primary Health Care – Primary health care is usually the first point of contact people have with their health care system, and ideally should provide comprehensive, affordable, community-based care throughout life.
Primary health care can meet the majority of a person’s health needs for the course of their life. Health systems with strong primary health care are needed to achieve universal health coverage.
Yet many countries do not have adequate primary health care facilities. This neglect may be a lack of resources in low- or middle-income countries, but possibly also a focus in the past few decades on single disease programs. In October 2018, WHO co-hosted a major global conference in Astana, Kazakhstan at which all countries committed to renew the commitment to primary health care made in the Alma-Ata declaration in 1978.
In 2019, WHO will work with partners to revitalize and strengthen primary health care in countries, and follow up on specific commitments made by in the Astana Declaration.
Vaccine hesitancy – The reluctance or refusal to vaccinate despite the availability of vaccines – threatens to reverse progress made in tackling vaccine-preventable diseases. Vaccination is one of the most cost-effective ways of avoiding disease – it currently prevents 2-3 million deaths a year, and a further 1.5 million could be avoided if global coverage of vaccinations improved.
Measles, for example, has seen a 30% increase in cases globally. The reasons for this rise are complex, and not all of these cases are due to vaccine hesitancy. However, some countries that were close to eliminating the disease have seen a resurgence.
The reasons why people choose not to vaccinate are complex; a vaccine advisory group to WHO identified complacency, inconvenience in accessing vaccines, and lack of confidence are key reasons underlying hesitancy. Health workers, especially those in communities, remain the most trusted advisor and influencer of vaccination decisions, and they must be supported to provide trusted, credible information on vaccines.
In 2019, WHO has ramped up work to eliminate cervical cancer worldwide by increasing coverage of the HPV vaccine, among other interventions. 2019 may also be the year when transmission of wild poliovirus is stopped in Afghanistan and Pakistan. Last year, less than 30 cases were reported in both countries. WHO and partners are committed to supporting these countries to vaccinate every last child to eradicate this crippling disease for good.
Click here for Deadly Diseases currently affecting humans Globally -
Know more about viruses –
Viruses are microscopic organisms that exist almost everywhere on earth. They can infect animals, plants, fungi, and even bacteria. Sometimes a virus can cause disease so deadly that it is fatal. Other viral infections trigger no noticeable reaction. A virus may also have one effect on one type of organism, but a different effect on another. This explains how a virus that affects a cat may not affect a dog.
Viruses vary in complexity. They consist of genetic material, RNA or DNA, surrounded by a coat of protein, lipid (fat), or glycoprotein. Viruses cannot replicate without a host, so they are classified as parasitic.
They are considered the most abundant biological entity on the planet.
Few facts on viruses –
Here are some key points about viruses.
- Viruses are living organisms that cannot replicate without a host cell.
- They are considered the most abundant biological entity on the planet.
- Diseases caused by viruses include rabies, herpes, Ebola, and Coronavirus.
- There is no cure for a virus, but vaccination can prevent them from spreading.
Dengue – Dengue, a mosquito-borne disease that causes flu-like symptoms and can be lethal and kill up to 20% of those with severe dengue, has been a growing threat for decades.
A high number of cases occur in the rainy seasons of countries such as Bangladesh and India. Now, its season in these countries is lengthening significantly (in 2018, Bangladesh saw the highest number of deaths in almost two decades), and the disease is spreading to less tropical and more temperate countries such as Nepal, that have not traditionally seen the disease.
An estimated 40% of the world is at risk of dengue fever, and there are around 390 million infections a year. WHO’s Dengue control strategy aims to reduce deaths by 50% by 2020.
HIV – The progress made against HIV has been enormous in terms of getting people tested, providing them with antiretrovirals (22 million are on treatment), and providing access to preventive measures such as pre-exposure prophylaxis (PrEP, which is when people at risk of HIV take antiretrovirals to prevent infection).
However, the epidemic continues to rage with nearly a million people every year dying of HIV/AIDS. Since the beginning of the epidemic, more than 70 million people have acquired the infection, and about 35 million people have died. Today, around 37 million worldwide live with HIV. Reaching people like sex workers, people in prison, men who have sex with men, or transgender people is hugely challenging. Often these groups are excluded from health services. A group increasingly affected by HIV are young girls and women (aged 15–24), who are particularly at high risk and account for 1 in 4 HIV infections in sub-Saharan Africa despite being only 10% of the population.
This year, WHO will work with countries to support the introduction of self-testing so that more people living with HIV know their status and can receive treatment (or preventive measures in the case of a negative test result). One activity will be to act on new guidance announced In December 2018, by WHO and the International Labour Organization to support companies and organizations to offer HIV self-tests in the workplace.
Ebola – Ebola is a rare but deadly virus that causes fever, body aches, and diarrhea, and sometimes bleeding inside and outside the body. As the virus spreads through the body, it damages the immune system and organs. Ultimately, it causes levels of blood-clotting cells to drop. This leads to severe, uncontrollable bleeding.
This virus is scary, but it’s also rare. You can get it only for direct contact with an infected person’s body fluids. The disease was known as Ebola hemorrhagic fever but is now referred to as the Ebola virus. It kills up to 90% of people who are infected.
Coronavirus – Coronaviruses (CoV) are a large family of viruses that cause illness ranging from the common cold to more severe diseases such as Middle East Respiratory Syndrome (MERS-CoV) and Severe Acute Respiratory Syndrome (SARS-CoV). A novel Coronavirus (CoV) is a new strain that has not been previously identified in humans.
Coronaviruses are zoonotic, meaning they are transmitted between animals and people. Detailed investigations found that SARS-CoV was transmitted from civet cats to humans and MERS-CoV from dromedary camels to humans. Several known Coronaviruses are circulating in animals that have not yet infected humans.
Common signs of infection include respiratory symptoms, fever, cough, shortness of breath, and breathing difficulties. In more severe cases, the infection can cause pneumonia, severe acute respiratory syndrome, kidney failure, and even death.
Standard recommendations to prevent infection spread include regular hand washing, covering mouth and nose when coughing and sneezing, thoroughly cooking meat and eggs. Avoid close contact with anyone showing symptoms of respiratory illness such as coughing and sneezing.

Click here for Health Issues Specific to Women’s Health -
While both men and women contract various conditions, some health issues affect women differently and more commonly. Furthermore, many women’s health conditions go undiagnosed and most drug trials do not include female test subjects. Even so, women bear exclusive health concerns, such as breast cancer, cervical cancer, menopause, and pregnancy. Women suffer higher heart attack deaths compared to men. Depression and anxiety exhibit more frequently among female patients. Urinary tract conditions present more often in females, and sexually transmitted diseases can cause more harm to women. Among the conditions that present most frequently in women, the following eight illnesses pose considerable health risks.
Heart Disease
In the United States, heart disease causes one in every four deaths among women. Although the public considers heart disease a common issue among men, the condition affects males and females nearly equally. Yet, only 54 percent of women realize that heart disease is the top health condition threatening their gender. In the United States, 49 percent of all consumers suffer from high blood pressure, high cholesterol, or smoke; factors that contribute to heart disease.
Breast Cancer
Breast cancer, which typically originates in the lining of the milk ducts, can spread to other organs and is the most aggressive cancer affecting the global female population. The condition presents more among female populations in developed nations due to their extended life spans.
Initially, women afflicted with breast cancer may develop breast lumps. Most breast lumps are non-threatening, but it is important for women to have each one checked by a care provider.
Ovarian and Cervical Cancer
Many people are not aware of the differences between ovarian and cervical cancer. Cervical cancer originates in the lower uterus, while ovarian cancer starts in the fallopian tubes. While both conditions cause similar pain, cervical cancer also causes discharge and pain during intercourse.
While ovarian cancer presents extremely vague symptoms, the condition is very complex. Finally, Pap smears detect cervical but not ovarian cancer.
Gynecological Health
Bleeding and discharge are a normal part of the menstrual cycle. However, added symptoms during menstruation may indicate health issues, and unusual symptoms, such as bleeding between menstruation and frequent urinating, can mimic other health conditions.
Vaginal issues could also indicate serious problems such as sexually transmitted diseases (STDs) or reproductive tract cancer. While care providers might treat mild infections easily, if left unchecked, they can lead to conditions such as infertility or kidney failure.
Pregnancy Issues
Pre-existing conditions can worsen during pregnancy, threatening the health of a mother and her child. Asthma, diabetes, and depression can harm the mother and child during pregnancy if not managed properly.
Pregnancy can cause a healthy mother’s red blood cell count to drop, a condition called anemia, or induce depression. Another problem arises when a reproductive cell implants outside the uterus, making further gestation unfeasible. Fortunately, obstetricians can manage and treat common and rare health issues that emerge during pregnancies.
Autoimmune Diseases
Autoimmune disease occurs when body cells that eliminate threats, such as viruses, attack healthy cells. As this condition continues to escalate among the population, researchers remain baffled as to why the condition affects mostly women. While many distinct autoimmune diseases exist, most share symptoms such as:
- Exhaustion
● Mild fever
● Pain
● Skin irritation
● Vertigo
Most of the autoimmune system rests in the stomach. Duly, many who suffer from this condition have resorted to natural healing practices, such as:
- Consuming less sugar
● Consuming less fat
● Lowering stress
● Reducing toxin intake
However, the best defense against autoimmune disease is early detection.
Osteoporosis
Osteoporosis weakens bones, allowing them to break easily. Several factors can cause the condition that occurs mostly in women, such as:
- Age
● Alcohol consumption
● Certain prescriptions
● Genetics
● Lack of exercise
● Low body mass
● Smoking
● Steroid use
To detect the condition, care providers measure bone density using an X-ray or ultrasound diagnostic. While no cure exists for osteoporosis, care providers can prescribe treatment to impede illness progression, which might include dietary supplements, healthy lifestyle choices, or prescription medication.
Depression and Anxiety
Natural hormonal fluctuations can lead to depression or anxiety. Premenstrual syndrome (PMS) occurs commonly among women, while premenstrual dysmorphic disorder (PMDD) presents similar, but greatly intensified, symptoms. Shortly after birth, many mothers acquire a form of depression called the “baby blues,” but perinatal depression causes similar – but much stronger – concerns, emotional shifts, sadness, and tiredness. Perimenopause, the shift into menopause, can also cause depression. No matter how intense the symptoms, care providers can provide relief with a prescription or therapeutic treatments.
Health Technology for Women
Soon, new technologies will emerge to assist care providers in treating women’s health conditions. Researchers have developed innovative medical treatments, such as a patient operated device that prepares women for breast reconstruction using carbon dioxide instead of needles and a blood test that can detect whether gestation has started outside of the fallopian tubes. Other developing medical technologies include an at-home, do-it-yourself Pap smear, and a test that determines pregnancy using saliva as a sample.
Women can lower the risk of cancers and other common illnesses with healthy habits and regular care provider visits. However, in many underserved communities, nurse practitioners (NPs) and nurse midwives fill the shortage created by a lack of care providers while covering service areas encompassing far too many clients. As America’s health care needs increase, care provider organizations will need many more NPs to ensure positive health outcomes for women in these communities.

Click here for How to tackle global health crisis -
Healthcare leaders around the world are familiar with the term “public health crisis”. From possible pandemics to the impact of obesity, our approach has been limited to reacting to the problem, not addressing its root cause.
This has become a paradox in healthcare. More than 50% of the world lives with chronic disease. Take the US, where chronic diseases, the majority of which are the result of decades of unhealthy behavior, impact 75% of seniors and account for 71% of the more than $3 trillion spent on healthcare.
99% of disease management is in the hands of individuals and their families.
The global population of the oldest seniors, 80 years of age or older, is expected to triple, to 446.6 million people, by 2050. Combined with the 50% of the world’s population that lives with chronic diseases today, this will certainly challenge healthcare systems around the world.
Healthcare leaders worldwide must shift from reactive, episodic care to managing health holistically, where the focus is helping people change their lifestyles so they can live healthier lives. Here are three initiatives healthcare leaders worldwide can adopt.
A. Intervene at the intersection of health and lifestyle –
It’s no secret that it’s difficult for doctors, patients, and caregivers to change unhealthy behavior, and patients’ personal circumstances, that lead to chronic conditions.
To have an influence, health insurance providers must be present at the intersection of health and lifestyle. Social determinants of health – such as food insecurity, social isolation, and loneliness that hinder an individual’s ability to alter unhealthy behavior – can be directly addressed at this juncture.
Insurance companies governed by the government of respective countries should take action at the intersection of health and lifestyle with what could be called Bold Goal: that the communities served will be 20% healthier because they can make it easy for people to achieve their best health.
They can partner with local food banks to learn about food insecurity and how screening for it in medical clinics could help, work with grocery stores and primary care physicians ( PHC) to address diabetes, nutrition, and health literacy, which has helped reduce the number of unhealthy days.
Yet these improvements are also dependent on care access. Increasing care access, and making it easier for people to obtain affordable care, is important, especially for care in the home. With aging populations impacting many countries, technology advancements that enable telehealth and remote monitoring will help caregivers stay connected to the loved ones they care for, as well as their clinical teams.
Care in the home is not only the preferred location for a person living with multiple chronic conditions; it’s also a lower-cost setting. By intervening at the intersection of health and lifestyle, they can help people make behavior changes while still living in their communities.
B. The transition from volume to value –
The unhealthy behavior and sedentary lifestyles adopted by societies worldwide have had a significant impact.
But there is a solution. In a value system, the physician is reimbursed not for the services, but for the patient’s health. The primary care physician plays the central role, including the coordination of care provided by specialists. This role enables the PHC ( Primary Health Centers ) to identify redundancies, such as multiple drug prescriptions. That helps slow disease progression and lower costs, making life easier for the patient and their caregiving team.
While physicians are embracing the value-based model with aligned incentives, a recent study of Family Physicians detailed barriers, from lack of staff time to a lack of resources to report, validate and use data that have not budged over the last few years.
Despite these barriers, physicians can partner and embrace the value-based model and the results for all members.
While value-based care reimburses healthcare providers based on the patient’s optimal health, physicians need real-time data that enables them to help correct unhealthy behavior to achieve these results.
C. Achieve interoperability in a digital age –
When you have interoperable workflows and systems, physicians, hospitals and health plans are all working together in managing the patient’s health, which leads to a better physician/patient relationship and sets the foundation for early intervention.
In an interoperable system, physicians have real-time, personalized information based on patient health and financial claim data that’s easily and securely shared via an Electronic Health Record (EHR). Physicians use EHRs to identify and intervene in moments of influence, such as proactively informing a patient his or her unhealthy behavior is leading to diabetes.
Technology will keep disrupting care, but it won’t solve everything. By incorporating technology as an element of the holistic approach, one that is designed to address unhealthy behavior and social determinants at the intersection of health and lifestyle through personalized data, chronic disease progression can be slowed down across the world.